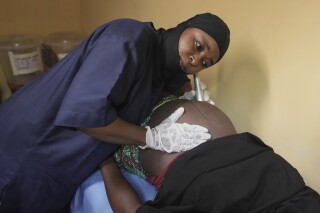
ABUJA — Nigeria’s community midwifery programme is significantly improving maternal and newborn health outcomes in conflict-affected rural communities of Yobe State, a new study has revealed.
The research, conducted by the EQUAL Research Consortium and unveiled in Abuja, found that community-trained midwives are strengthening staffing levels and expanding access to lifesaving services in underserved primary healthcare centres.
Dr Emilia Iwu, Senior Technical Adviser at the Institute of Human Virology Nigeria (IHVN), disclosed the findings at the close-out and dissemination meeting of the five-year multi-country EQUAL project implemented across Nigeria from July 2021 to April 2026.
According to the study, community-trained midwives were nearly twice as likely as graduates of the basic programme to originate from rural communities and to remain working in primary healthcare facilities serving their own areas.
Within six months of graduation, 67 per cent of trainees had secured employment, while 64 per cent were deployed directly to underserved rural health facilities across Yobe.
Service delivery indicators were also strong. Nearly all the midwives reported conducting deliveries, 90 percent provided antenatal care, and 70 percent offered family planning services, significantly widening access to essential maternal and reproductive healthcare.
The study projected that modest increases in midwife-delivered interventions could prevent 22 percent of maternal deaths and 23 percent of neonatal deaths statewide.
However, Iwu warned that systemic challenges could undermine long-term sustainability.
She cited irregular salaries, political interference in postings, poor working conditions and limited career progression as major threats to retaining skilled personnel in rural areas.
Attrition, she noted, is highest within the first five years of practice, as many midwives migrate to better-paid urban or NGO positions offering improved security and welfare.
Despite recorded progress, gaps persist in newborn care, patient communication and emotional support.
Women surveyed cited financial hardship, family influence and cultural barriers as reasons for delayed care-seeking.
The researchers recommended harmonised salaries, improved facility security, mental health support, protected funding and formal recognition of midwife roles within the civil service structure.
Dr Ebere Anyachukwu, Health Adviser at the UK Foreign, Commonwealth and Development Office, reaffirmed the United Kingdom’s commitment to supporting maternal and newborn health in fragile settings, stressing that women and infants in conflict-affected communities face the greatest survival risks.
Dr Emmanuel Udontre, representing the Registrar of the Nursing and Midwifery Council of Nigeria, commended the research team for producing solution-driven evidence.
Mrs Hadiza Sabo, Provost of Shehu Sule College of Nursing Sciences, described the findings as an eye-opener, highlighting excessive workloads, low pay and weak career structures as hidden pressures within the workforce. She called for a state-level service scheme to formalise career progression and improve retention.
She clarified that while council-regulated midwives hold certified qualifications, traditional birth attendants remain unregulated, limiting their formal integration into Nigeria’s healthcare framework.